A lot of people have opinions about this subject, and it is one that I’m passionate about. I agree that opiates are bad, and people shouldn’t be started on them if at all possible. The government is waging a war against opiates and they are hard to get from any doctor now. No one will prescribe opiates if they can help it.
But there needs to be a second plan for those of us who have been on opiates for 35 years and need them to survive. Those of us whose bodies are completely reliant on them to function. Not everyone who takes opiates is an addict. I’ve never been an addict and I don’t consider myself one, even though I know I need the medication to deal with my chronic pain.
Addiction is in your mind. It’s when you can’t go without something. People can be addicted to anything. Diet coke, ice cream, nasal spray, Carmex… Anything you put into or on your body that changes the way you feel, can be addicting. Not always a chemical addiction, but an addiction nonetheless.

Like many, I was started on opiates as a young teenager with ovarian cysts and migraines. That was back when they’d throw vicodin at you for pain. Here, numb it with this. My tolerance throughout the years has grown to something astronomical, unbelievable even, especially when nurses can’t understand why my pain can’t be touched. I take medication daily for my chronic pain that is a partial agonist. I’ve been taking it (Subutex) for 10+ years. It doesn’t “kill” the pain, but numbs it enough to make it tolerable on a steady basis. No ups or downs, I don’t “feel” any pain relief when I take it. And it blocks all other opiates, though it does have an opiate base. HOWEVER, it is a medication that’s also given to heroin addicts to cease their addiction (though they take it for days to months–not 10 years), and every time I see a doctor or nurse that’s new to me, they always treat me in a manner that is judgemental, and can sometimes be called cruel.
For most people, the drug can be stopped three to four days before surgery and the opiates given will work.It is even said that a high enough dose of opiates should supercede the Subutex. However, I have a problem. That doesn’t work for me. I have to wait MUCH longer to feel any pain relief.
I AM the 1%.
First, I tried stopping the medication three days before a procedure–and felt the whole thing.
Then I tried one week. Same result.
During the next procedure, I had ceased my medication one and a half weeks before the event [a procedure called a Discogram, and has nothing to do with dancing] and the sedation didn’t work at all. As the doctor was working on my neck, I asked him if they were going to give me something for the pain, and he informed me that they’d done so about ten minutes ago. I felt the entire procedure, every needle puncturing a disc in my neck, awake and talking to the doctor. The process of this procedure was to put four needles in my neck at the same time, one in each disc.
I had to remain awake because they would pump liquid into each disc to see if it stayed in the nucleus, or flowed out, meaning the disc was broken. My job was to tell them when I couldn’t stand the pain anymore. They went in through the front of my neck and had to repeat the fourth needle several times as it kept getting caught on my collarbone. They were finally in and we discovered that three of the four discs were broken.
The doctor kept telling me to hold on, and that he would have the nurses “take care of me” when we were done. I sat, nearly rocking in pain, and waited for pain relief in the recovery room behind a fabric curtain with my husband. Since the sedation didn’t work, there’s nothing they could do for me, but I didn’t know that. All I knew was that the doctor said they’d take away all the pain they’d just put me through. My husband and I heard two nurses meet outside my room, and one said to the other, “She’s a Subutex patient–don’t give her ANYTHING.”

I was livid. Even if I WAS an addict, they have high tolerances for pain medication, and they do feel pain. In fact, the longer you are on opiates, the more new pain nerves grow, causing even more legitimate pain. More importantly, they have just as much right to pain relief as anyone else. And it will take MORE medication for them, not less. Nurses cannot make a judgment call like that when they don’t know the story. But now it’s that way with all opiates.
But I ask you, what are the people like me supposed to do? Just get over it? That’s not in the cards for me. My fourth spinal fusion with a decompression laminectomy is scheduled for May 29th, 2020. In order to get pain relief from the medication to work while I’m at the hospital, I must stop my current medication and go through withdrawal, as well as deal with ALL my pain, for 21 days, until it’s completely out of my system. Why 21 days? That is how long it takes for me. I know, I know, it should take 3 days. My doctor is on your side. Though he’s been my doctor the whole time, he refuses to believe that it takes my body that long.

The doctors believe that the shelf life of the medication should have it out of my system in four days max. When you take Buprenorphine (or Subutex), your body makes metabolites called norbuprenorphine. These metabolites are why a person can test positive for fourteen days after ceasing the medication. Apparently, it takes me another week (hence, approximately 21 days). When you look at it that way, it doesn’t seem so implausible.
The issue is, as long as those metabolites remain in my body, I am completely blocked from all other opiates–all sedation, all pain medication.
Again, I have tried to stop the medication a few days before, I’ve tried to stop it one- and two-and-a-half weeks before procedures, and both the last time [and this time] it took twenty-one days to feel any pain relief from another opiate. The first time, after three days off the Subutex, I was given four shots of fentanyl in the ER, but felt no relief. They couldn’t believe I felt no pain relief, but I sat there, quivering in pain and deadpan asked, “Do I look like a person who’s just had four shots of fentanyl?” They said no, but were confused.
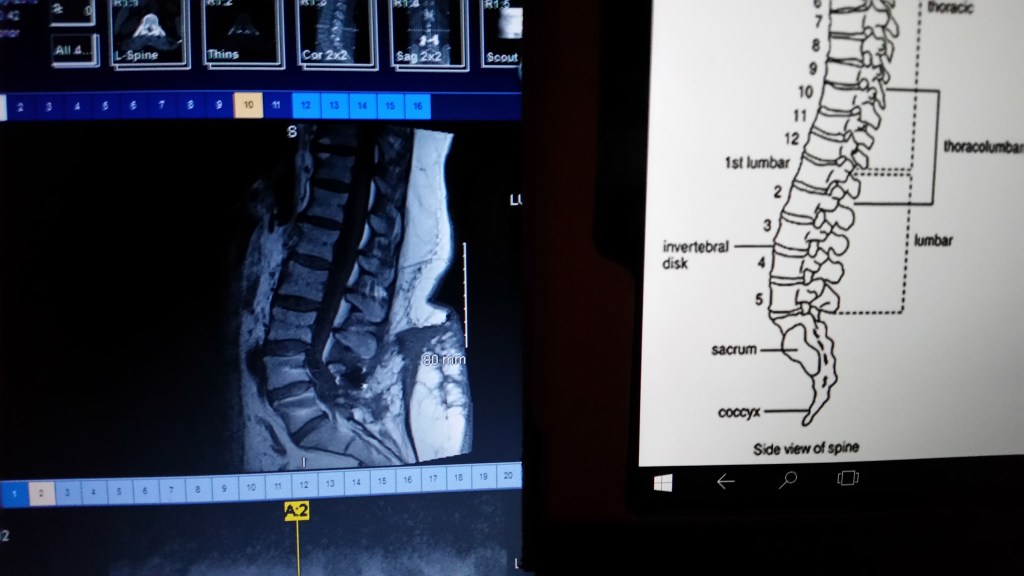
So where is my chronic pain? Mostly in my back, some in my neck. Through the years, the pain has changed. I’ve had my ovaries removed and the migraines have been fine. But I inherited some issues from my sweet dad that keep me in a constant state of chronic pain. I have the spine of a 70 to 80-year-old, in a 46-year-old body.
The diagnosis: There are bone spurs growing (spinal stenosis) from my neck to tail, as well as degenerative disc disease. Two thoracic discs are herniated, three of four discs in my neck are broken, I have lumbar osteoarthritis, kyphoscoliosis (which means the spine curves incorrectly from side to side, but also front to back), my neck curves the wrong direction (reverse cervical lordosis), I have a spinal stimulator, and I’m fused from L2/L3/L4/L5 and next month I can add L5/S1. The levels that really need the surgery are at the top of the fusion (T11/T12/L1), but they are dangerous to do as it is lung and cord level, plus the bone may crumble (I have osteoporosis as well). But the discs have degenerated so much in the last year that both of those top levels are pressing against the thecal sac (which is the sleeve that holds your spinal cord). I will likely need that surgery soon. Probably next year. Then I will be fused from the bottom up to T10. That doesn’t make me happy.

I am not imagining my pain. It is real and it is horrible. One of the nurses told me during my last surgery–when the morphine pump didn’t work at all–that I’ve screwed my body.
“If you broke a bone, or were in here for a car accident, we wouldn’t be able to help you at all,” she said. “There is nothing we could give you until after you went through 3 weeks of withdrawal.”
I replied, “I’m here now and you can’t help me at all.”
I deal with more pain on a daily basis than some people feel in their whole life and my poor family gets caretaker fatigue.
“What’s wrong?” they ask.
“Nothing,” I say.
“Oh, are you in pain?”
“Always. I’m sorry.”
“No don’t apologize. You just have ‘pain face’ and I was just concerned.”
“Okay.”
*Two hours later*
“Hey, you okay?”
“Yep.”
“What’s wrong?”
“Nothing.”
“You sure?”
“Yeah. I’m just hurting.”
“Again?” they ask.
“Still.”
And I feel so lame being the one who hurts all the time. I can’t do anything. I can’t work an outside job. (But I haven’t worked enough in my lifetime to receive any benefits, they tell me.) I edit books to keep my mind off my pain. And now that I have to stop my medication before the surgery and get it out of my system, I asked my doctor to prescribe (again) a bottle of percocet for the pain from the time my meds are gone until the surgery.
But because of the opioid epidemic, no one wants to give them to me. Everyone agrees I shouldn’t have to be in pain, but no one wants to be the one to prescribe the opiates. My GP refused and sent me to a special doctor, and he won’t give me any either. He told me to go back to the GP and ask again. I did and was sent back. The surgeon hasn’t answered my calls and only gives out Tramadol, which to a person like me, works about as well as baby aspirin. I wouldn’t even fill it. No, I probably would because it would be all I could have. (But I wouldn’t feel any pain relief.)
[Update 5/24/20: The surgeon is the only one who would prescribe me pain relief until the surgery. My actual doctors have left me to deal with the pain on my own, and my own Subutex doctor does not believe it takes more than four days. He keeps saying, “It works this way for all my patients…” I told him, “It doesn’t work for me and I AM one of your patients.” He is ignoring me until I go back on the Subutex, calling my requests “ridiculous.”]
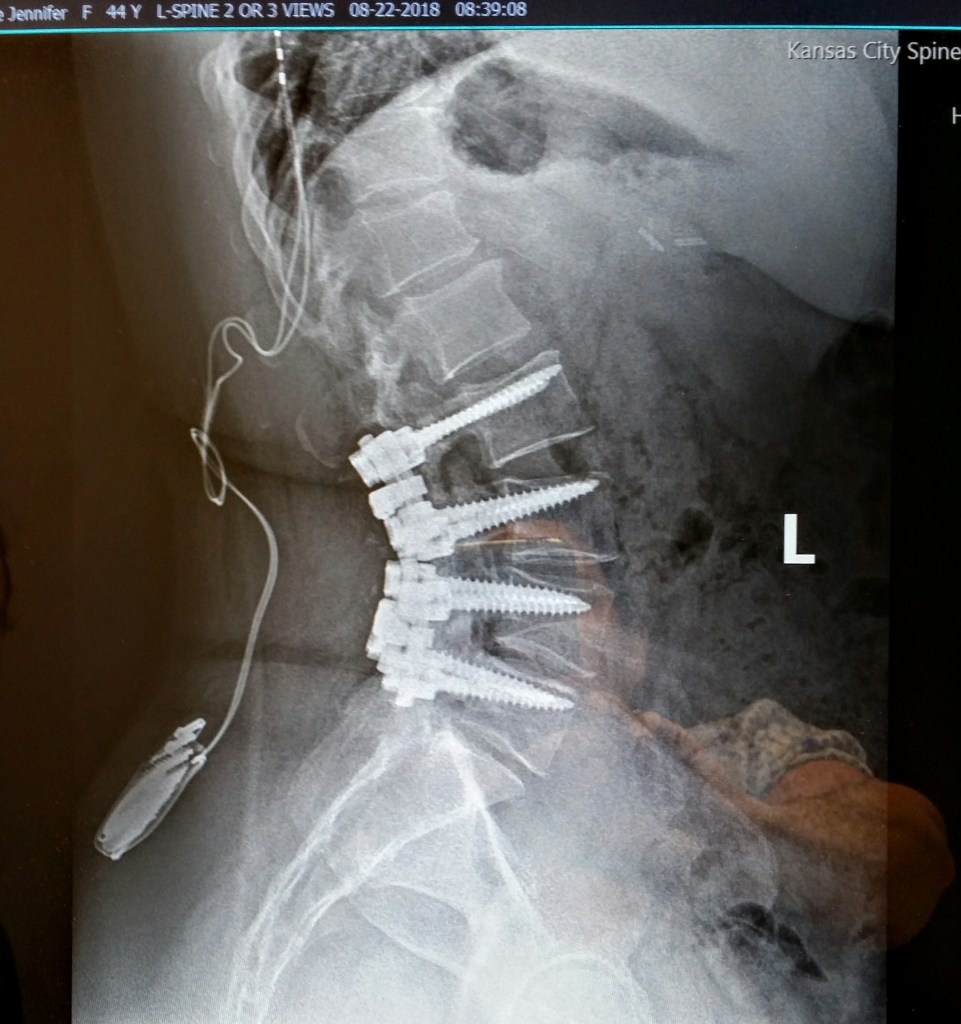
Sometimes, people stare at me and some make comments because I have a handicapped placard and no wheelchair. But they don’t see how much effort it takes me to walk. They don’t see the spinal stimulator implanted in my hip that’s wired to the pain center of my brain. That’s the contraption in my hip, and I charge it every few days through the skin. After nine or ten years, they’ll cut out the battery and replace it.
A lot of people ask about the spinal stimulator. It is NOT pain relief. It is meant to be a distraction from the pain. When it’s “on” it is similar to the pins-and-needles that you feel when your foot falls asleep, or like a TENS machine, if you’ve ever felt one. When the stimulator’s on (most of the time), my body buzzes like that from my ribcage down. Yes, EVERYWHERE. It takes some getting used to. It feels like wearing electrified pantyhose. The idea is this: you know when you break your arm, all you can think is, “Ow, my arm. Ow, my arm.” Then, if someone were to activate your electrified pantyhose, you’d be like, “Ow, my arm. Whoo! My tingles. Ow, my arm, whoo, my tingles…”
In theory, your brain can’t fully focus on two pains at the same time. So you still feel all your pain, you just ALSO feel this prickling all over that should take some of the brainpower away from feeling so much of the pain. It doesn’t really work. I mean, if you broke your arm and I kicked you in the shin, they would both still hurt. Maybe one at a time, but you’d feel it all. When I forget to charge the battery through my skin, the stimulator sometimes dies and I don’t realize it. Then–when I turn it back on–I feel a split second of pain relief and it feels so good to have the tingles back because I’ve gotten so used to it. But that’s about it for pain control.
At this point, I use whatever I can to make the pain tolerable; walking, cold, heat, brace, gel seat cushion, good shoes… Unfortunately, I also need opiates. Especially when I’m about to have surgery. I’m not an addict–there is no reason why I shouldn’t have them at this point–but because of the epidemic, I am out of luck. It will be very hard for me to keep up with the blog throughout May/June, but I will do my best. I know everyone is wanting to see how the books do, so I will try, but please forgive me if the posts are shorter.
I have had some luck with the AMS ads and I’m still learning. So I will tell you all about that next week, and give you the update on our WIP. I got it back from my editor on Friday and I’m dying to look, but I haven’t had the time. It’s making me so excited. I have chosen some great agents that I targeted well and I can’t wait to do the final edits and send it out.
Please support me in my fight by realizing this epidemic isn’t a black and white issue. It needs to have two parts: not starting people on opioids, and taking care of the people who are already using and need them. I live in Kansas and we don’t even have legal medicinal marijuana to fall back on. We are sandwiched between Colorado, Oklahoma, and Missouri–all legal. If you are going to take our opiates, at least give us alternative pain relief.

Sign your Kansas petitions for legalization. Here’s a link: https://sign.moveon.org/petitions/legalize-the-use-of-marijuan
Unfortunately, Kansas doesn’t work the same way with petitions as Missouri and Oklahoma, but if we show Governor Kelly that there’s a need, maybe she will acquiesce.
All of you have a great week and I will see you next weekend with book news galore. Thanks for letting me rant and include my two cents. And if you have a cause you are passionate about, let us know in the comments and give us a link to support you!
[Update 6/6/20: The Surgery went well. The disc between L5 and S1 was completely crushed and being forced out the side. So the surgeon said he fashioned a cage in that fusion (It’s the little cylinder below that looks like a bullet). I’ve only ever had Steri-strips to close the wound, but this time they used staples–25 staples–and I’ll having them removed was fun. Of course, the first thing I did was pull out half of the bottom staple, but the others held. They itch like crazy. I’m trying to work, but I’m only up for about four hours at a time, then sleep for three–between medication doses. I got a fabulous anesthesiologist this time who’d just had training on chronic pain patients and knew to give me extra medication, and I did beautifully. I’m taking lots of walks around the block with my walker, like a granny. Lol. The opiates make me very emotional, as well. I will take them as a normal patient would, then go back to my Subutex doctor. If I didn’t need him, I’d leave though, because his behavior throughout this ordeal has been unfathomable to me, and uncaring at best. Thank you for all your support! I’ll keep you updated.]


Have a great week. Until next weekend, Keep Writing!
~jenn




I’m so sorry that you are in so much pain, Jenn. My prayers are with you.
LikeLiked by 1 person
Thanks, Karen. I will take all the prayers I can get!
LikeLiked by 1 person